
Prologue:Previous and our latest laboratory results showed that this disease is caused by filamentous biofilm bacteria (FBB) and subsequently also promotes various secondary infections. Most likely, in the case of an FBB infection, there is a causal relation to stress-related pre-existing conditions due to an insufficient, endocrine HPA stress axis. In particular, noticeable by an overreactive immune system (stress-induced), whereby an excess of histamine, prostaglandins, leukotrienes, cytokines, or T-cells are detectable.
Which in the later course of the disease almost always cause hyperallergic and multi-inflammatory reactions. Often also blood clots, thrombosis, heart attacks and ultimately cancer. In the initial phase of infection by filamentous biofilms (FBB), a clear medical diagnosis is extremely difficult. Since a bacterial infection with biofilms is generally a new dimension of disease, it should force physicians to rethink.
Especially with this disease, various bacteria of different kind, which are embedded in a biofilm, can also exchange DNA with each other via plasmids. Furthermore, filamentous growth (three-dimensional biofilm) can spread by means of an extracellular, polysaccharide matrix (biofilm streamers) consisting of polysaccharides (cellulose), lipids, various proteins and within endospores or bacterial protoplasm is included with the nucleus and nucleic acid and the DNA. Some information and images about biofilm streamers - see links below:
Source: Some Information and Images about Biofilm-Streamers:
Source: Bacterial solutions to multicellularity: a tale of biofilms, filaments and fruiting bodies
This rare filamentous form of biofilm, which spreads rather fungus-like to colonize the environment, has an evolutionary advantage over individual bacterial accumulations, e.g. free-living bacteria or so-called planktonic cells, which can only spread obligate and partially glide in a limited location, e.g. in any moisture.
In addition, they have extremophilic properties and have found a survival niche at the boundary between wet and dry areas, and are mostly multiresistant to common antibiotics. Furthermore, such biofilm bacteria have been for a long time evolved into multicellular organisms. Such bacteria do not come from Mars, but from the soil! Biofilm infections are under the radar and could probably be a cause of many diseases!
Biofilm streamers cause catastrophic disruption of flow with consequences for environmental and medical systems
These bacteria are not typical pathogens per se, perhaps opportunistic, so that they would not only infect immunocompromised individuals, but rather highly sensitive individuals are affected with a stress-related, over-shooting immune system, healthy people can serve as carriers, but they don't get sick, or not so quickly.
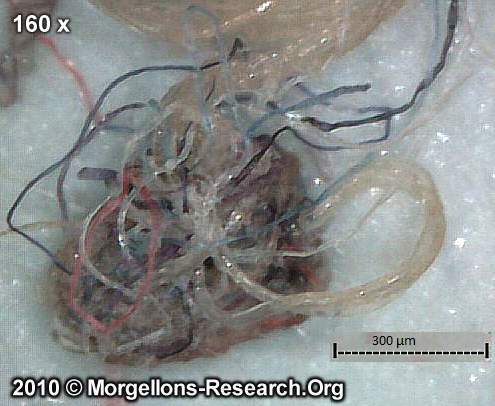
Biofilm filament bundle
In the later course of the disease the HPA-stress axis will collapse and producing even less stress hormones (cortisol, noradrenalin, etc.), unable to counteract properly the stressful situation anymore, as a result of a pituitary gland and following adrenal gland insufficiency.
These bacteria are now unfortunately also increasingly marketed as bacteria for agriculture by biotech companies, such as biological pesticides, plant growth promoters (nitrogen binding), horizontal gene transfer (glyphosate plants), etc.
Laboratory tests:
These laboratory tests should mainly be done if the disease has been present for a longer time!
Infection parameter:
If one is infected with such bacteria, it will arise in the further course of the typical symptoms as with other bacterial infections, but by means of serology, no signs of infection can be measured by common infectious parameters (IgA, IgM, IgG, IgE, etc.), as these bacteria are embedded in a biofilm and would therefore not present antigens. The granulocyte levels in the blood may be reduced, or normal, or also strongly reduced in the later course of the disease.
Also, a disturbed or decreased hormone balance due to long-term stress (somatropin, serotonin, cortisol, DHEA, norepinephrine) may be present. Functional tests CRH/ACTH trigger hormones, as well as haemoglobin levels, serum albumin and ESR 32 should also be investigated. Sometimes only leukocytes or CRP (C-reactive protein) levels are slightly increased or the levels of cytokine, histamine in the blood initially increased slightly at the beginning of the disease and later borderline.
Procalcitonin is inconspicuous, just as applied blood cultures by default, are also negative. Even with PCR tests, you can't get any further, because you don't have the naked bacterium in your blood. Thus, biofilm bacteria usually escape the usual laboratory examination, which is a disaster for the respective patient.
Biofilm cultivation:
Mainly cultures of biofilm and its filamentous extensions (streamers) or tissue samples should be made on MacConkey, blood/urea, broth, nutrient-rich boullions, or bacilli agar (NGA) at 26 - 28° Celcius (78,8 °F - 82,4 °F Fahrenheit) for 6-8 days to detect all involved bacteria inside biofilms, e.g. from the Bacillus cereus group or various other agrobacteria such as Rhizobium radiobacter, A. vitis, B. megaterium, B. subtilis, B. pumilus, B. mycoites, B. licheniformis, B. circulans, or bacteria like Sphingomonas xenophagum, Pseudomonas or Stenotrophomonas maltophilia.

Biofilm mass growing out from a black filament (wildlife form)
Genotype identification should not necessarily be done by PCR tests, but rather via 5'-end gene sequencing via a 16S rRNA test (cost $50-80 dollars), to prove e.g. bacilli or C58, A. rhizogenes K1026 or K84 (old. A. radiobacter K84), A. radiobacter CFBP 2414T, or A. vitis LMG 8750T (vini/viticulture, wine-growing). Even an infrared spectrometry, or an immunofluerence test, can detect rare microorganisms even in previous, negative cultures. It is also possible to search specifically for elevated values of polysaccharides (biofilm) through special laboratories.
Evidence of microscopic examinations usually shows only cellulose filaments with slime produced by these bacteria for attachment to any host organism, and are confused with clothing fibres, since they also consist of polysaccharides like cellulose (cotton fibers).
This disease is more likely to be considered a systemic disease and is not a skin disease per se, as the biofilm usually spreads first from the intestine to the bloodstream, organs and much later on the skin. Later, the immune system reacts more and more with hyperallergic and multi-inflammatory reactions to the bacterial proteins (proteolytic digestive enzymes) or by-products (ammonium), and at least in the later course of the disease some increased inflammatory parameters can be detected, such as prostaglandins, leukotrienes, cytokines, T cells and amplified histamine.
In terms of skin symptoms, there are sometimes more and sometimes fewer pustules, swellings, blisters or redness, which resemble insect bites. Probably due to the bacterial enzyme release with subsequent allergic reaction of the skin (histamine release, etc.), which is not an IgE-induced reaction. Likewise, these bacteria themselves also produce histamine, which can later lead to histaminosis or histamine intolerance, and ammonium, which can lead to convulsions and other neurological damage.
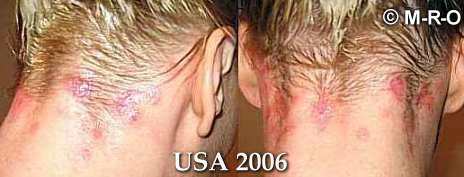
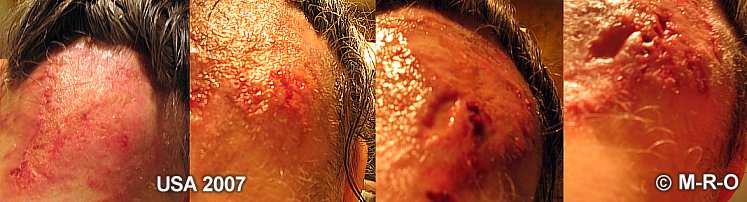
Antrax-like wounds
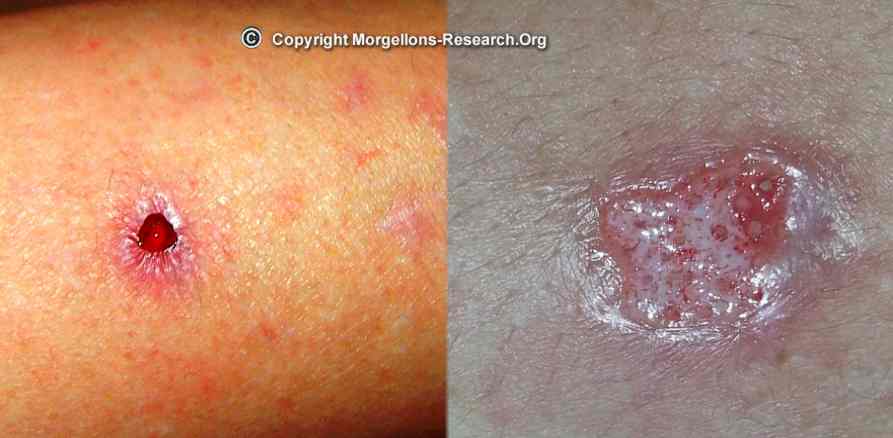
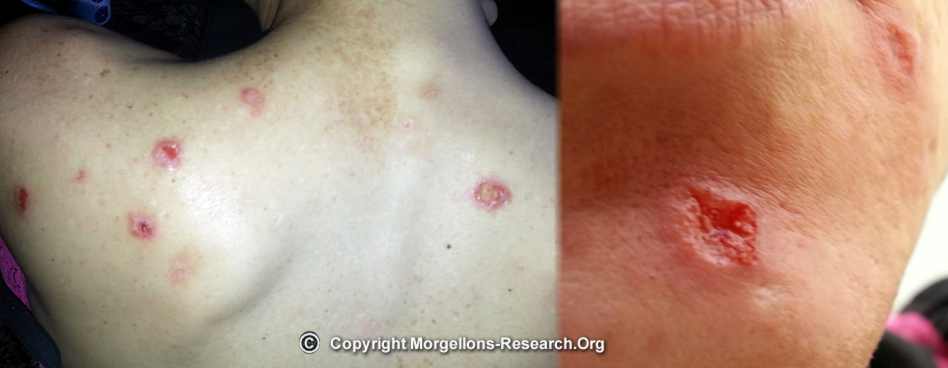
By spraying on the skin with a chili cream (dermatologist) or aloe vera, one can usually make infestation areas visible, because then, as with acne, small pustules etc, are created. Even with a black light lamp you can see glassy fibers on the skin, which do not always come from clothing abrasion. You can also apply milk or oils to the cleansed skin to propel out some threads.
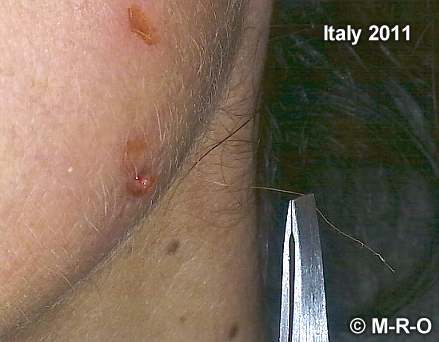
More precise microscopic skin examinations by a light microscope and skin scrapes, or an adhesive tape flap taken directly from the skin surface, provide more clarity. Since usually some threads/fibers, as well as a gel-like mass or granules stick to it. Typical infestation sites can also be found in the areas of the eyes, nose, mouth and ears. These samples should be cultivated, as mentioned above.
A survey of the patient about his or her circumstances would also be useful in order to determine whether, for example, possible re-infection via pets, partners, laundry, etc., should be ruled out. All bacteria are located in a single biofilm, which in nature can spread filamentously in the soil and twisted with fungal hyphae or plant roots for a symbiosis. Hence the formation of filaments is related due to stress because of a nitrogen deficiency or temperatures higher than 35 degrees Celcius.
Unfortunately, such infections caused by various agrobacteria (e.g. Rhizobium radiobacter, B. megaterium, etc.) are still unknown to most physicians and human laboratories, although there are already sufficient medical case-studies.
Source: Agrobacterium as human pathogen
Source: Agrobacterium and relation to Morgellons
Source: Common Plant Vector A. tumefaciens injects Genes into Human Cells
This contradicts my findings, as most of the patients stated that they did not actually have a noticeably weakened immune system. Rather they had traumatic and stressful times before the infection and some in turn actually suffered from immunosuppressive pre-diseases such as cancer, bacterial infections such as Lyme disease, etc. These diseases also cause stress symptoms in the body with constant elevated stress hormones and histamine, but with lowered immunoglobulines.
See the following source information on agrobacterial hospital germs:
http://www.sciencedirect.com/science/article/pii/S1201971208000878
http://www.seq.es/seq/0214-3429/30/1/chanza25nov2016.pdf
http://www.microbiologyresearch.org
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC130740/
https://www.ncbi.nlm.nih.gov/pubmed/8086552/
https://academic.oup.com/cid/article/38/1/149/355862/
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4985768/
http://cid.oxfordjournals.org/content/38/1/149.full
http://www.ncbi.nlm.nih.gov/pmc/articles/PMC3133165/
http://www.nature.com/bmt/journal/v26/n1/full/1702470a.html
http://path.upmc.edu/cases/case98/dx.html
Rhizobium
radiobacter, or otherwise called Agrobacterium tumefaciens
or A. radiobacter,
A. vitis,
etc., so always the same bacterium only with other properties, can
produce systemic diseases, and is, besides Bacillus megaterium,
probably one of the main pathogens of this biofilm disease. B. megaterium can
cause antrax-like cutaneous wounds.
However, it is possible to check in advance whether there is also an active infection by spirochetes. The fact is, if not all, e.g. Lyme disease antigen bands are detectable, there can also be a completely different bacteria that can cause cross reactions (band 41) by similar antigens. But spirochetes are also used by the pesticide industry as biological insecticides and the clinical symptoms could be interpreted as Lyme disease!
BACTERIA, SPIROCHETES, AND RICKETTSIA AS INSECTICIDES
https://nyaspubs.onlinelibrary.wiley.com/doi/abs/10.1111/j.1749-6632.1973.tb32749.x
Bridges, fillings and tooth loss, and often also muscle and joint pain,oedema, nerve inflammation, low or elevated blood pressure, confusion, forgetfulness, fibromyalgia, headache, eyelash and hair loss. Also with the first signs of autoimmune diseases. This reinforces the conclusion that such diseases can actually be caused by microbial infections. There is a lot of research on such diseases, but what happens when they are also triggered by biofilms that cannot be easily detected?
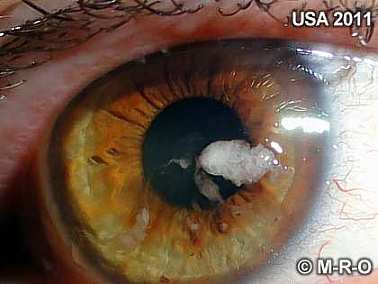
In some sufferers, even after years, there are just few skin symptoms, but only an infestation of the sinuses, nose, ears and especially the eyes and surrounding tissue. A worse or blurred view is typical, with later development towards cataracts.
-----------------
------------
In general, it can be said that cutaneous and subcutaneous symptomsresult from biofilm filaments and integrated bacteria, which cause skin lesions resulting from enzyme release. Many skin symptoms are not only caused by Rhizobium radiobacter, or Bazillus megaterium, B. cereus etc., but also overlap with secondary infections (opportunistic bacteria or dermatophytes).
This biofilm can be divided into short filaments or small blebs and washed through the lymphatic system into all physical areas and finally into the skin pores, where there in the skin pores, develops into longer filaments (coils, fuzzballs). Sometimes in the skin pores several colourful filaments (tyrosinase-related colour production) are intertwined and then appear as thread-balls, so-called black specks.
Since the biofilm adheres to the hair root, it grows out with the hair on the skin surface in order to get back later into the skin by enzyme release. This results in the typical allergic skin symptoms (pustules, blisters). A short haircut is very helpful to reduce the adhered biofilm mass.
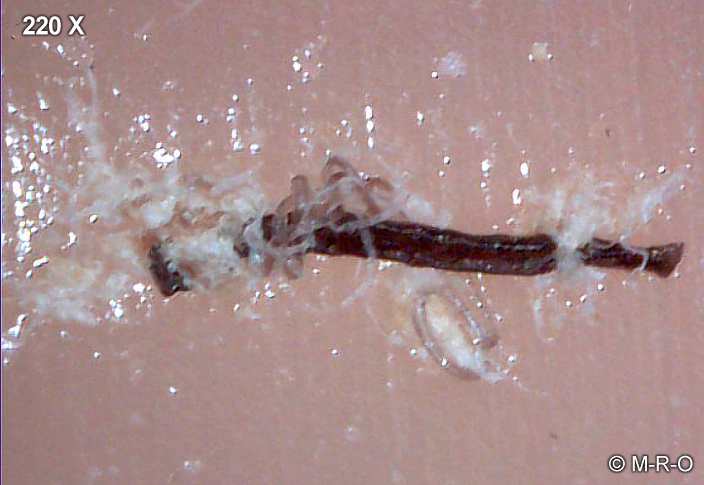
Small biofilm filaments and blebs growing out with hairs
Some filaments can also be transferred to other individuals or objectsby sweating out on the skin through simple body contact. Infectious contact is thus by sweat, skin and hair, blood, urine, tear fluid, stool, and other bodily fluids! Many visitors of my site claimed they likely have Morgellons. However, they had no filaments that could be found anywhere, or typical signs of biofilm infection, but similar skin symptoms (acne?).
Not all skin symptoms or disease are related to Morgellons. A differential diagnosis could be preceded by scabies and some other bacterial/mycotic infectious skin diseases. These include in particular very similar mycotic infections such as with Phaeoacremonium parasiticum, Pityrosporum folliculitis or Coccidioides immitis and some dermatophytes. As well as protozoa infections of e.B. Pythium insidiosum or skin diseases such as Prurigo or Urticaria, or endo- and subcutaneous cygomycosis (mold infection), - these can cause similar skin symptoms.
A histopathological examination is indicated in all cases. Additional co-infections may occur later due to the multiplication of opportunistic pathogens (candida, enterobacteria, viruses, etc.) due to a partially weakened immune system (low immunoglobulins) also due to kidney inflammation and cystitis. Immunoglobulins are increasingly washed out by a constant urge to urinate. But also other pathogens may be involved, which previously had contact with the mentioned filaments/biofilm in nature, intestines, etc., and remained glued to them or were integrated into the biofilm.
Pre-existing conditions:
Early traumatic experiences and dramatic strokes of fate are characteristic for all sufferers. Mainly these earlier (post-traumatic stress) and also current traumas, or latent infections and the resulting permanent stress hormone distributions along with physical consequences (disbalancing of the vegetative nervous system and immune system, pituitary insufficiency, HPA stress axis) are causative to get these diseases with negative influence on the immune competence of the affected persons.
Autoimmune diseases, multiple inflammations and, as a result, cancer had developed in many patients in the late stages. 29% died of aggressive pancreatic cancer! But also a poor diet, or predispositional factors such as diabetes mellitus, cancer and a previous, false corticosteroid therapy, nervous diseases, viral diseases, pre-existing autoimmune diseases such as Hashimoto, metabolic diseases, thyroid disease, as well as surgical trauma, mercury fillings removals, can cause stress situations and be decisive or trigger for infection with these pathogens. Increased nitrogen levels!
The biofilm can be first colonized in the mouth-nose area as well as inthe scalp area or on the skin. A larger blister formation or a rash can occur only after 3-4 days or already on the first day of infestation, depending on the sweat formation and the current virulence (food deficiency of bacteria) of the biofilm filaments. Often you can see skin lesions/pustules around the eye areas/head, whereby also the eyebrows and eyelashes are infested and often also fail.??? In the morning, the eyelashes are sometimes glued. Skin lesions tend to form more often at typical sweat zones.
Later also at other physical extremities, such as around the eyebrows, eyelids and upper eyelids, eyelashes, ears, nose, lips, tongue, gums, mucous membranes in the mouth and nose area, in the eyes, elbows, nipples, knees, joints, feet, toes, vaginal area, cervical area, scrotum. Also around the nipples, at the neck and at the décolletage, at the belt line, the shoulders, the back of the hand, between the fingers and all other areas that produce sweat.
Some skin areas also resemble dermatoses or eczema, but the skin is already massively infiltrated with the biofilm, which grows predominantly subcutaneously and also constantly reacts to internal and external influences, such as water, acids, alcohol, pressure. Also by pressure points of the hands, which lie on the body or head or by lying longer on a part of the body (side or shoulders, back), a sweat layer is automatically formed in between, which also influences the lymphatic system and there can manifest more skin symptoms.
If these filaments are swallowed directly, the symptoms may be delayed or even absent for a long time. Since these microorganisms then only spread in the large and small intestine for the time being and later, due to various factors, aim for an expansion towards the bloodstream or subcutaneous areas and subsequently encapsulated in the nerve tissue or connective tissue, mucous membranes, and much later after stress conditions of the patient break out there again. If we are talking about migrating biofilms, then possibly also resident fungi (Candida) and enterobacteria, etc. could be dragged further into the bloodstream, or involved in a DNA transfer to pass on resistance via plasmids.
According to an M-R-O survey, about 17% of sufferers (mostly in warmer areas) are additionally burdened by infestations with various insects, which also leads to initial misdiagnosis. Insects, as is known, are increasingly attracted by nitrogen/ammonium. When this bacterial biofilm settles in the human epidermis and the sweat glands, the metabolism of these nitrogen-binding bacteria (urease, ammonium) may then attract more all sorts of insects and also leads them to lay their eggs in the skin. At the same time, the nitrogen utilization of these bacteria and the conversion (ammonium/ammonia) can lead to nerve inflammation, cramps and nerve damage, etc.
German Site Copyright © M-R-O 2021 Contact